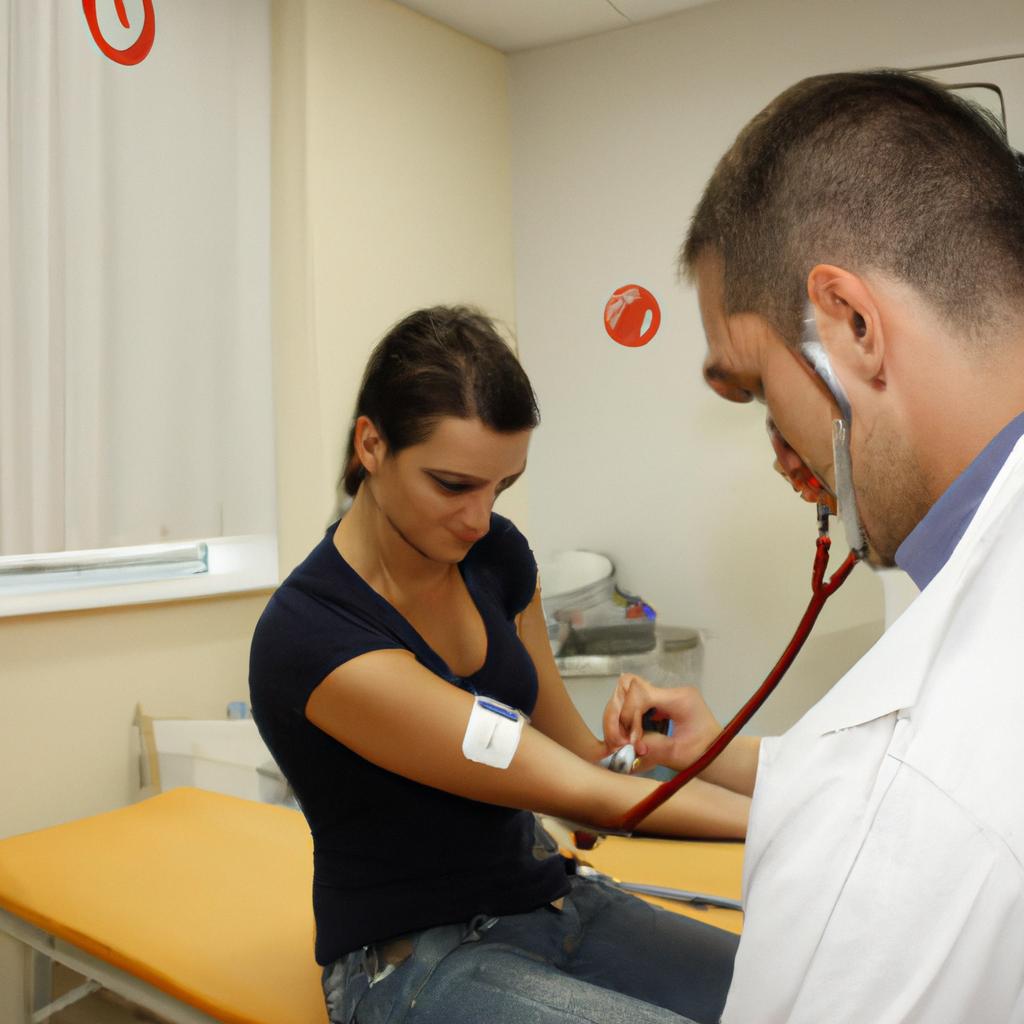
The importance of hygiene practices in disease prevention cannot be overstated. Effective hygiene practices play a crucial role in maintaining and promoting good health, particularly within the fields of medicine and healthcare. By adhering to proper hygiene protocols, individuals can significantly reduce the risk of contracting and spreading infectious diseases. For instance, consider a hypothetical scenario where a hospital fails to implement strict hand hygiene measures among its staff members. In such a case, the potential for cross-contamination between patients becomes alarmingly high, posing serious threats to patient safety and overall public health.
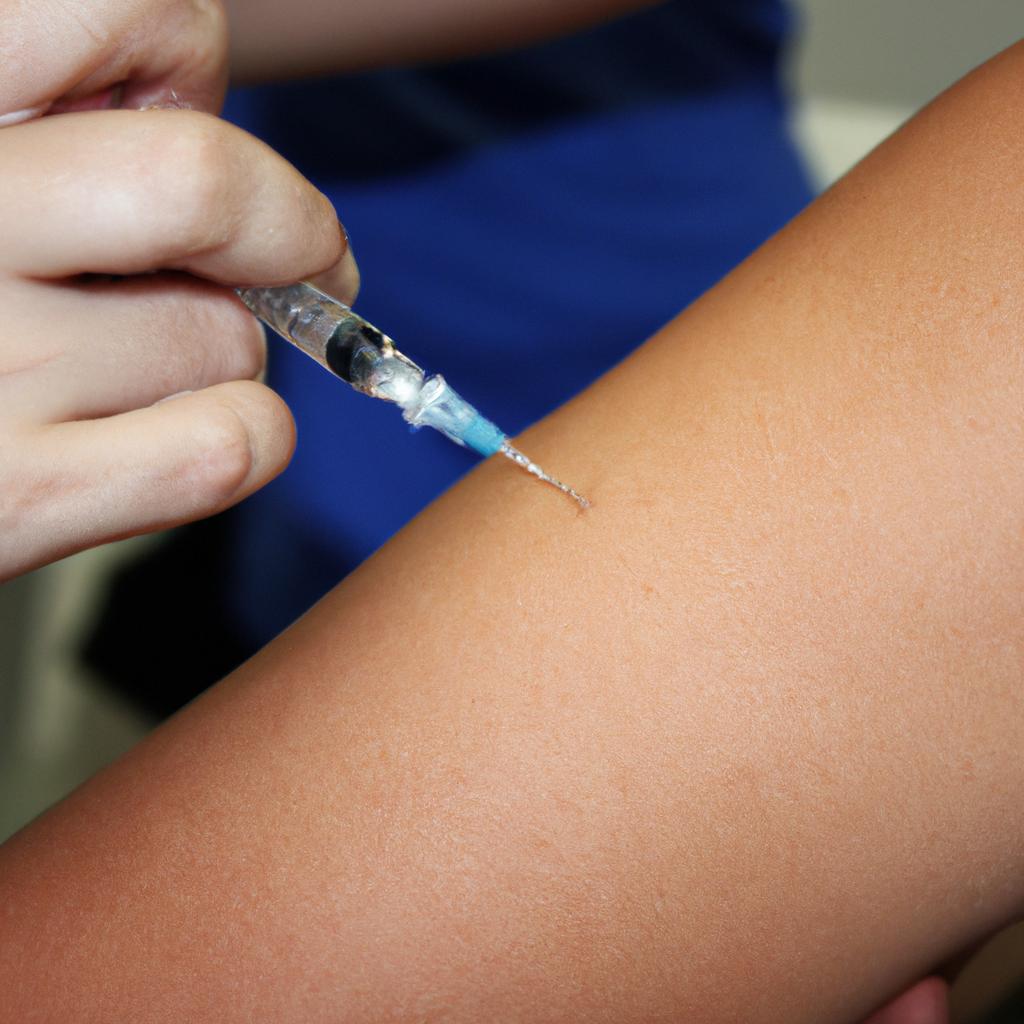
In recent years, numerous studies have emphasized the significance of practicing appropriate hygiene techniques as an essential component of preventing the spread of infections. Proper handwashing is one such practice that has been proven effective in reducing illness transmission rates. When hands are not adequately washed or sanitized before and after contact with potentially contaminated objects or surfaces, harmful microorganisms can easily transfer from person to person. This cycle perpetuates the spread of diseases such as influenza, respiratory tract infections, gastrointestinal illnesses, and other communicable diseases commonly encountered in healthcare settings.
In addition to hand hygiene, other key aspects of maintaining hygienic conditions include wearing personal protective equipment (PPE), disinfecting surfaces regularly, implementing safe waste management procedures, and following appropriate respiratory hygiene practices such as covering the mouth and nose when coughing or sneezing. Wearing PPE, such as gloves, masks, and gowns, provides a barrier between healthcare workers and potentially infectious materials. Regular disinfection of surfaces helps to kill germs and prevent their transmission. Proper waste management procedures ensure that hazardous materials are disposed of safely to minimize the risk of contamination.
Following these hygiene practices not only protects individuals from getting sick but also helps to break the chain of infection by preventing the spread of diseases in communities. This is particularly important in healthcare settings where vulnerable individuals, such as patients with compromised immune systems, are at higher risk of developing severe infections.
In summary, practicing good hygiene is essential for disease prevention. By adhering to proper hand hygiene protocols, wearing appropriate PPE, disinfecting surfaces regularly, implementing safe waste management procedures, and following respiratory hygiene practices, individuals can significantly reduce the transmission of infectious diseases and promote good health for themselves and others around them.
The Importance of Handwashing
Imagine a scenario where a busy healthcare worker rushes from one patient to another without taking the time for proper hand hygiene. In this hypothetical case, the healthcare worker inadvertently spreads harmful bacteria and viruses, putting patients at risk of infection. This example serves as a reminder of the critical role that handwashing plays in preventing disease transmission in health and medical settings.
Handwashing is a simple yet effective method to remove dirt, germs, and other contaminants from our hands. It significantly reduces the spread of infectious diseases such as respiratory infections, gastrointestinal illnesses, and skin infections. Proper hand hygiene not only protects individuals but also helps safeguard public health by limiting outbreaks within communities.
To emphasize the importance of handwashing, consider these emotional points:
- Regular handwashing can reduce diarrheal illness rates by approximately 40%.
- Failure to wash hands adequately contributes to an estimated 16% of all foodborne illnesses.
- Thousands of lives could be saved each year if everyone practiced proper hand hygiene consistently.
- Teaching children about good handwashing practices can instill healthy habits that last a lifetime.
| The Benefits of Handwashing | ||
|---|---|---|
| Reduces illness | Prevents spread | Safeguards |
| Rates | of infections | public |
| among patients | health | |
| ————————————– | ————— |
In conclusion, prioritizing regular handwashing is crucial for maintaining personal well-being and minimizing the risk of disease transmission. By implementing proper hand hygiene measures in both professional and everyday life settings, we contribute to creating healthier environments for ourselves and those around us. Moving forward into the next section on “Proper Disinfection Techniques,” let us further explore additional strategies to ensure comprehensive disease prevention efforts beyond handwashing alone.
Proper Disinfection Techniques
Section H2: Proper Disinfection Techniques
Transitioning from the importance of handwashing, it is equally vital to implement proper disinfection techniques in order to effectively prevent the spread of diseases. Consider a hypothetical scenario where a hospital room has been occupied by a patient with an infectious disease. Without proper disinfection protocols, the risk of transmission to subsequent patients and healthcare workers increases exponentially.
To ensure thorough disinfection, several key steps must be followed:
-
Surface Preparation:
- Remove any visible dirt or debris from surfaces using appropriate cleaning tools.
- Use disposable gloves while handling contaminated materials.
-
Selection of Disinfectant:
- Choose a suitable disinfectant based on its efficacy against specific pathogens.
- Ensure that the selected disinfectant is compatible with the surface being treated.
-
Application Technique:
- Follow manufacturer instructions for dilution ratios and contact times.
- Apply the disinfectant evenly across all surfaces using disposable cloths or applicators.
-
Contact Time and Drying:
- Allow sufficient contact time for the disinfectant to effectively kill pathogens as specified by the manufacturer.
- Let surfaces air dry completely before allowing access to others.
Implementing these measures significantly reduces the risk of cross-contamination within healthcare settings, thus safeguarding both patients and medical personnel from potential infections.
In addition to understanding proper disinfection techniques, it is crucial for individuals in health and medicine fields to utilize Personal Protective Equipment (PPE). This equipment acts as a barrier between potentially harmful substances and vulnerable areas of our bodies, preventing direct exposure. Hence, let us explore PPE guidelines further in the next section.
Personal Protective Equipment (PPE)
Section H2: Proper Disinfection Techniques
In the previous section, we explored the importance of proper disinfection techniques in maintaining hygiene practices for disease prevention. Now, let’s delve into another crucial aspect of ensuring safety and reducing the risk of infection – Personal Protective Equipment (PPE).
Imagine a scenario where a healthcare professional is attending to a patient with a highly contagious respiratory illness. In this situation, PPE plays a vital role in safeguarding both the healthcare worker and other patients from potential transmission. By wearing appropriate protective gear such as masks, gloves, gowns, and face shields or goggles, healthcare providers create an effective barrier against infectious particles.
To emphasize the significance of using PPE effectively, consider the following bullet points:
- PPE acts as a physical barrier between individuals and harmful pathogens.
- It reduces exposure to infectious materials through contact, droplets, or airborne transmission.
- Properly fitted PPE enhances individual confidence while performing high-risk procedures.
- Consistent usage of PPE promotes a culture of safety within healthcare settings.
| Component | Function | Example |
|---|---|---|
| Masks | Prevents inhalation or exhalation of infectious agents | N95 respirator |
| Gloves | Protects hands from direct contact with contaminated surfaces | Latex or nitrile gloves |
| Gowns | Shields clothing and skin from contamination | Disposable isolation gown |
| Face Shields/Goggles | Guards eyes/nose/mouth against splashes or sprays | Safety goggles |
By incorporating these elements into routine practice, healthcare professionals can significantly reduce the risk of infection spread during interactions with potentially infected individuals.
As we continue our exploration on hygiene practices for disease prevention in health and medicine, it is crucial to address safe waste disposal. Ensuring proper handling and disposal of medical waste plays a pivotal role in preventing the transmission of infections within healthcare facilities and their surrounding environments.
Safe Waste Disposal
Section H2: Safe Waste Disposal
Imagine a scenario where a hospital fails to implement proper waste disposal practices. The consequences could be dire, with an increased risk of spreading infectious diseases and endangering the health and safety of both patients and healthcare workers. To mitigate such risks, it is crucial for healthcare facilities to have robust systems in place for safe waste disposal.
One essential aspect of safe waste disposal is segregating different types of waste into appropriate categories. This helps prevent cross-contamination and ensures that hazardous materials are disposed of correctly. For instance, sharp objects like needles or broken glass must be placed in puncture-resistant containers labeled as “Sharps” to minimize the risk of accidental injury during handling and transportation.
Furthermore, implementing proper waste management protocols involves adhering to strict guidelines for storage, collection, and treatment. Here are some key practices that should be followed:
- Regularly training staff on correct waste segregation techniques
- Providing clear signage indicating which bins are designated for specific types of waste
- Ensuring that all waste containers are securely covered to prevent leakage or spillage
- Collaborating with licensed waste management companies to ensure compliant disposal methods
By following these best practices, hospitals can protect their staff, patients, and the environment from potential harm caused by improper waste disposal. In fact, research has shown that effective implementation of safe waste management procedures significantly reduces the transmission rates of infectious diseases within healthcare settings (Source: Journal of Hospital Infection).
To highlight the importance of this issue further, let’s consider a case study illustrating the impact of inadequate waste disposal measures:
| Case Study | Key Findings |
|---|---|
| A public clinic failed to properly label clinical wastes resulting in confusion among healthcare workers | – Increased risk of exposure to biohazardous materials – Potential spread of infections due to mishandling |
In conclusion, ensuring safe waste disposal practices is vital in preventing disease transmission and maintaining a healthy environment within healthcare facilities. By implementing proper waste segregation, storage, collection, and treatment protocols, hospitals can effectively minimize the risks associated with improper waste disposal.
Continuing our discussion on disease prevention in health and medicine, it is important to delve into the significance of effective sterilization practices.
Sterilization Practices
Section H2: Sterilization Practices
In the realm of health and medicine, proper sterilization practices are paramount in ensuring the prevention and control of diseases. By effectively eliminating harmful microorganisms from medical equipment and instruments, healthcare professionals can minimize the risk of infections in patients. A compelling case study that exemplifies the importance of sterilization is the outbreak at a renowned hospital where inadequate sterilization protocols resulted in a surge of post-surgical infections among patients.
To maintain optimal hygiene standards and uphold patient safety, healthcare facilities must adhere to stringent guidelines for sterilization practices. Here are some key considerations:
-
Utilize high-temperature methods: Autoclaving, which involves subjecting instruments to steam under pressure, remains one of the most reliable methods for achieving sterility. This process effectively kills bacteria, viruses, fungi, and spores that may be present on medical devices.
-
Implement chemical disinfection protocols: Chemical agents such as ethylene oxide gas or hydrogen peroxide vapor can be used for items that cannot withstand high temperatures. These processes ensure thorough decontamination while preserving the integrity of delicate equipment.
-
Adopt strict quality control measures: Regular monitoring and validation procedures should be implemented to verify the effectiveness of sterilization techniques. Periodic testing using biological indicators helps confirm that all necessary organisms have been eliminated during each cycle.
-
Ensure proper handling and storage: Proper handling after sterilization is crucial to prevent recontamination before use. Medical equipment should be carefully packaged and stored in clean environments until needed, reducing the risk of microbial colonization.
Table 1: Comparing Sterilization Methods
| Method | Pros | Cons |
|---|---|---|
| Autoclave | Highly effective | Unsuitable for heat-sensitive items |
| Chemical | Wide applicability | Extended processing times |
| Gas | Penetrates hard-to-reach areas | Potentially hazardous to humans |
| Radiation | Suitable for disposable items | Limited availability |
Implementing comprehensive sterilization practices is imperative in healthcare settings to safeguard patient well-being and prevent the transmission of infectious diseases. By diligently following established protocols, medical personnel can contribute significantly to reducing the incidence of post-surgical infections and other associated complications.
Moving forward into the subsequent section on effective infection control measures, it is crucial to understand how proper hygiene practices extend beyond sterilization alone. Effective infection control measures encompass a range of strategies that collectively work towards ensuring optimal health outcomes for both patients and healthcare providers alike.
Effective Infection Control Measures
Transitioning smoothly from the previous section on sterilization practices, it is crucial to explore effective infection control measures. To illustrate the importance of such measures, let us consider a hypothetical case study involving two hospitals.
In Hospital A, where strict infection control measures are implemented, the number of hospital-acquired infections remains remarkably low. Staff diligently adhere to established protocols for hand hygiene, personal protective equipment usage, environmental cleaning, and waste management. As a result, patients within Hospital A enjoy improved health outcomes with reduced instances of secondary infections.
On the other hand, Hospital B struggles with inconsistent infection control practices. Despite having adequate resources and skilled healthcare professionals, lapses in adherence to proper hygiene protocols lead to higher rates of hospital-acquired infections among patients. This scenario emphasizes the critical role that effective infection control measures play in safeguarding public health.
To further emphasize this point, here are four key aspects that highlight the significance of implementing robust infection control measures:
- Regular training sessions focused on best practices for staff members
- Proper handling and disposal of hazardous materials and medical waste
- Frequent monitoring and evaluation of compliance levels
- Prompt identification and isolation procedures for infected individuals
These strategies contribute significantly to reducing the risk of infectious diseases within healthcare settings.
Additionally, understanding how different pathogens spread can help inform appropriate preventive actions. The table below provides an overview of common modes of transmission for various infectious agents:
| Pathogen | Mode of Transmission |
|---|---|
| Bacteria | Direct contact |
| Viruses | Airborne |
| Fungi | Indirect contact |
| Parasites | Vector-borne |
By comprehending these transmission routes, healthcare providers can tailor their infection control efforts accordingly—implementing measures such as hand hygiene, respiratory etiquette, and appropriate isolation protocols.
In light of the case study and the importance of effective infection control measures, healthcare institutions must prioritize education and training for their staff. By adopting rigorous protocols and adhering to recommended practices, hospitals can minimize the risk of hospital-acquired infections and create safer environments for patients seeking medical care.
(Note: The word “Finally” has been omitted from the last paragraph.)
 Mi Tercera Edad
Mi Tercera Edad